I have in my blog An introduction to Life in Africa talked about my experience of arriving in Africa with a cholera vaccination one day over the 6 months protection promised, that is out-of-date by one day. I don’t think that I’ve had an injection for cholera since, rather relying on hygiene. The vibrio which causes cholera is present in the faeces of a sufferer and either spread by direct inoculation on soiled objects (eg hands or flies) or drinking water with infected faecal material in it.
Thus toilet paper, hand washing and boiling or sterilising affected water are the main protective mechanisms.
On the other hand without toilets or clean running water spread is rapid in developing countries.
People defecate near a water supply (eg creek), some faeces may spill into the creek or people wash their hands or bodies in the water. Further down the waterway someone drinks and ‘boom’.
Cholera gives extremely severe diarrhoea and a patient can die within 12 hours from dehydration.
Our home and hospital water supply was from the local creek.
As a medical service we were inundated with cases.
We set up 2 extra ‘hospitals’ one by ‘acquiring without consent’ a newly built un-occupied house in a village from which 14 people had died during the day before we set this temporary ‘hospital’ up. It was much bigger and better than the surrounding kraals with 5 rooms. We had to deal with the owner a few days later! The people were so terrified that they refused to bury their dead and left them out to be eaten by the hyenas. There we also set up a vaccination program under the shade of a huge tree not far away from the village. In this house/hospital patients lay on the floor as we had no beds and their bowel actions were handled by bed pans. The nurse and helpers who ran it deserved gold medals! No one died there, very serious cases were transferred to our major hospital. There are special cholera beds with holes under the buttocks with canvas funnels below to collect the massive diarrhoea in largish containers. We had none of these in either hospital so there was much work with very frequently used bedpans.

The second hospital was a large tent, usually used for celebrating weddings or funerals, set up next to our main hospital. The main hospital still had plenty of work. There were about 40 beds in the tent. A young 17 yo visiting Australian, while not medically trained, supervised the night watch. The local workers tended to find a place to sleep if there was a hiatus in work. The young man kept an eye on the IV drips and status and woke the workers if/as necessary.
We setup a vaccination program using senior primary school students to perform the intracutaneous injections. (A number of our primary school students were late teenagers or young adults who had previously had no education. They were seeking a basic 3R education.) This intracutaneous route was chosen because the volume of vaccine used was much smaller, and we had a limited supply. These older students were used to responsibility; and learned fast. This program was supervised by an American physiotherapist and they carried out over a hundred thousand injections in a number of sites around the area over 3 weeks. The tribal population was about a million.

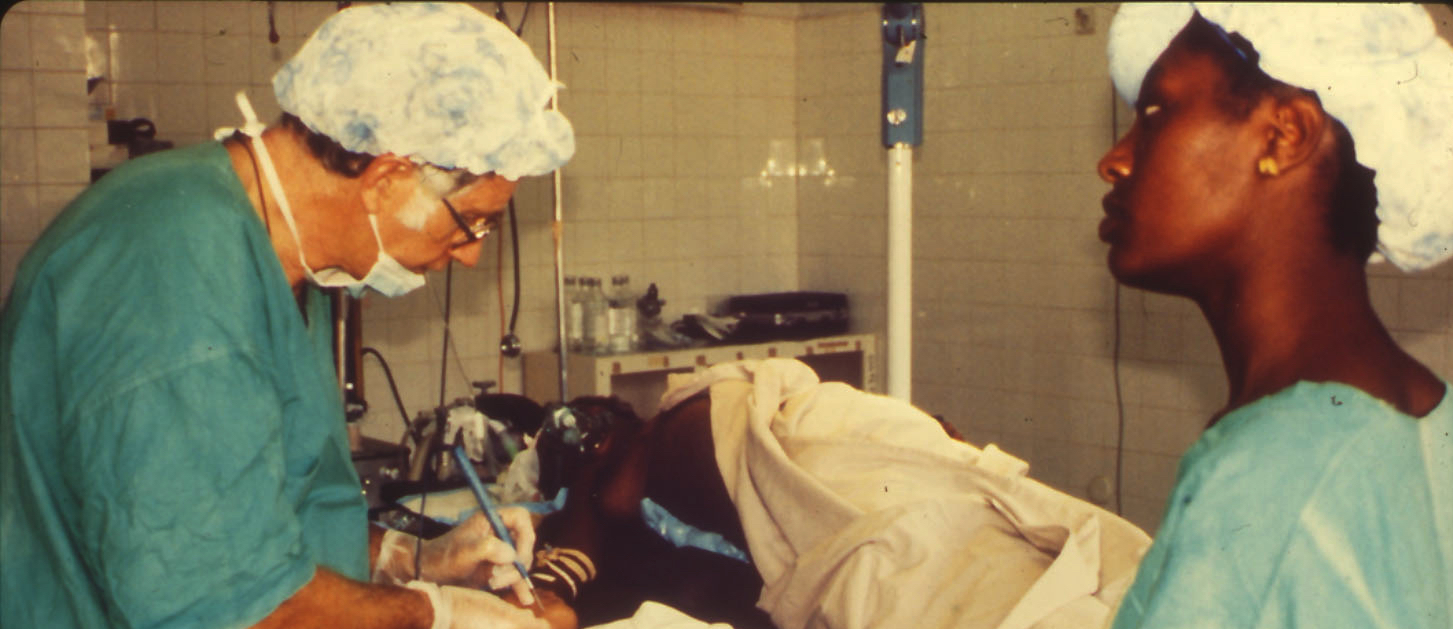
The bed above was typical of those being used in our University hospital in 2017. They are much better than what we had in our cholera tent!
Fortunately we were 2 doctors there at the time. The advantage was tempered a bit, however, as one of our sons was born during this time, a bit premature and fairly heavily jaundiced. My wife took him to the capital for advice and as an escape from the environment.
The government and WHO were very generous providing adequate antibiotics and a plane load of IV fluids. The plane landed in a field near the hospital.
We treated over 900 as inpatients within a month, without a death among those who arrived at the hospital alive. In addition those with milder symptoms were treated as outpatients within the hospital grounds.
Treatment was urgent and intense but in the appropriately treated the cure was rapid. The antibiotic we had was long acting sulphur. Patients needed sometimes up to 30 litres of IV fluid in the first 24 hours (keeping up with the diarrhoea) but after that it lessened quickly and we made them drink water from which the dirtiness had been settled out with alum and sterilised with chlorine. We had difficulty getting them to drink our ‘clean’ water. They said it had no taste. We bought 3 different cake colourings (red, blue and yellow) and coloured the water, lying I guess, and insisting that it was powerful medicine. In reality that was true for the dehydrated.
An interesting experience. I was went through a smallpox endemic at another time.
Dominic Cartier.
Continue reading “A brush with cholera”

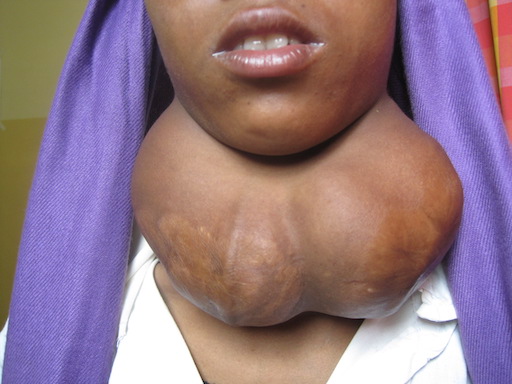 As I understand, the world record for the weight of a thyroid is 13Kg. This example maybe slightly more than a Kg which still weighs much more than the normal about 20Gm.
As I understand, the world record for the weight of a thyroid is 13Kg. This example maybe slightly more than a Kg which still weighs much more than the normal about 20Gm.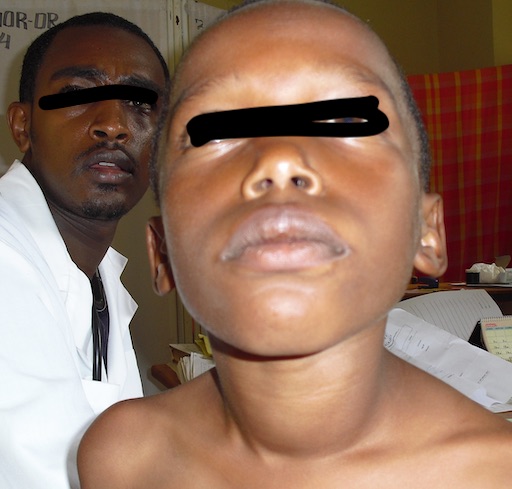 This small thyroid in a young teenage boy proved to be malignant. The post grad student in the picture has become a famous surgeon.
This small thyroid in a young teenage boy proved to be malignant. The post grad student in the picture has become a famous surgeon.