
(The house complex above was often the set up of a polygamous family. The Husband had the bigger house and each of his wives a smaller one.)
Tadessa was the second of the 3 teenagers who became part of our home -see A house full of teenagers. The first, Mesfin, was dealt with in Follow up on Mesfin of the ‘3 Teenagers’
Tadessa was much gentler than Mesfin but just as studious. I remember how they were taught English in High School. There were sentences with a or maybe two spaces, followed by a list of alternate words or phrases to put in the spaces. For instance there may have been a verb in several tenses and they had to choose the right one. In the evenings he would discuss the alternatives with my wife. Unlike me she is good at English. I remember him more than once stating that her answers had been marked wrong. When he had commented to the teacher that he lived with people whose first language was English and that he had checked his answers with them he was told that they obviously didn’t know English very well.
With Mesfin he was sent to school in Addis and went onto tertiary studies. He studied accountancy and administration. When they were leaving our area to go for further schooling in Addis their church friends gave them a party. It was joyous and memorable. Memorable to me in several ways – the music and singing (not the canned variety) were great, and the retelling of shared experiences was hilarious but, outstanding in my mind was that the catering was only dry bread and water; and they all appreciated it. My wife and I, invited as their ‘parents’ were spoiled. We had a coke and a fanta!
He worked with the training school attached to the Hamlin Fistula Hospital. Then with Samaritan’s Purse. He was in the Finance Department of the Korean Hospital in Addis Ababa. Now he is CEO of the work in Ethiopia of an American Mission.
This mission has built and runs a school for 1400 children in a poor area about 150 km. They provide 2 meals a day for the students. He still lives in the capital. From there he deals with the American heavies in the USA and the Government heavies in Addis, frequently travelling to the school to oversee its running. At the mission’s request he is planning to start a second school.
Over the years he has worked as a go-between for us dealing skilfully with government departments, whereas we would have bumbled our way through, and often have failed.
Perhaps the supreme example of this was when, after a 2 year battle to adopt our second Ethiopian son, he solved the question by marching into the senior officer in the case and saying “you know every legal requirement has been met. You’re only waiting for a bribe and this family don’t bribe. Say ‘yes’ and the case is finished. Say ‘no’ and we’ll take you to court”. He marched out of the office. Two days later he was called in to collect the signed papers. It is of interest that in the preceding few weeks a number of officials from other departments had been sacked for taking bribes.
He is married with 3 lovely boys. His wife is a nurse.
I’ve lent him money which he is repaying in part by helping educate a number of other children.

Dominic Cartier




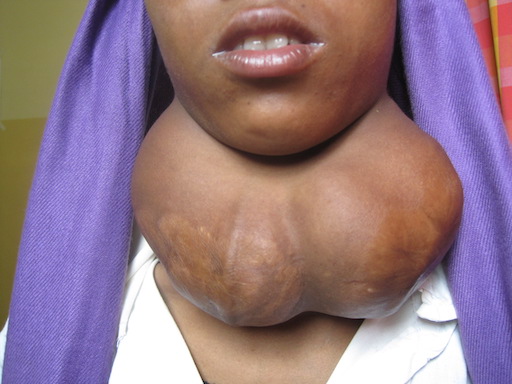 As I understand, the world record for the weight of a thyroid is 13Kg. This example maybe slightly more than a Kg which still weighs much more than the normal about 20Gm.
As I understand, the world record for the weight of a thyroid is 13Kg. This example maybe slightly more than a Kg which still weighs much more than the normal about 20Gm.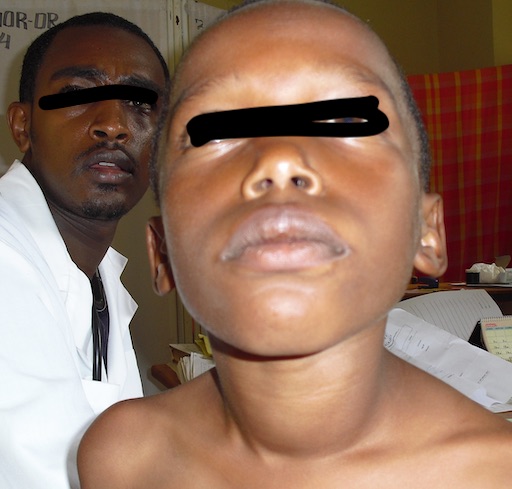 This small thyroid in a young teenage boy proved to be malignant. The post grad student in the picture has become a famous surgeon.
This small thyroid in a young teenage boy proved to be malignant. The post grad student in the picture has become a famous surgeon. Th
Th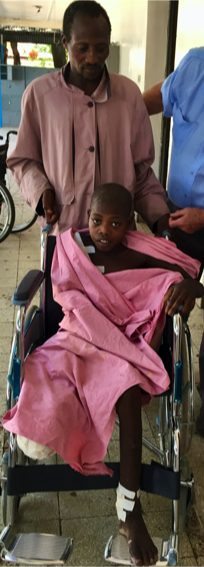 He survived this but soon developed tetanus. This is hard to treat anywhere but much more in an open ward with no intensive care specialists available – but we did. Besides the initial guillotine type amputation surgery he needed other refashioning and skin graft surgery. Early mobilisation is always attempted but how do you get one mobile if he has no armpit for a crutch and no leg on the same side? The hospital had a few wheel chairs for emergency use but none to be dedicated for a single patient. My wife and I fortunately had enough money to buy him a wheel chair which he loved. I retired when nearly 80 before the saga ended but we hadn’t solved the problem by any means. There is no social security in the country. Everything has to be paid for – so that even if it were possible to make an artificial above knee prosthesis learning to work without an arm to hold a crutch would be extremely difficult. He and his father could whizz around the cement paths of the hospital in the chair but when they went back into the mountains there would be mud and slush galore and probable no cement paths at all. I grew quickly to love both of them but I can’t even begin to imagine what life is like for them now.
He survived this but soon developed tetanus. This is hard to treat anywhere but much more in an open ward with no intensive care specialists available – but we did. Besides the initial guillotine type amputation surgery he needed other refashioning and skin graft surgery. Early mobilisation is always attempted but how do you get one mobile if he has no armpit for a crutch and no leg on the same side? The hospital had a few wheel chairs for emergency use but none to be dedicated for a single patient. My wife and I fortunately had enough money to buy him a wheel chair which he loved. I retired when nearly 80 before the saga ended but we hadn’t solved the problem by any means. There is no social security in the country. Everything has to be paid for – so that even if it were possible to make an artificial above knee prosthesis learning to work without an arm to hold a crutch would be extremely difficult. He and his father could whizz around the cement paths of the hospital in the chair but when they went back into the mountains there would be mud and slush galore and probable no cement paths at all. I grew quickly to love both of them but I can’t even begin to imagine what life is like for them now.